Can't go over it. Can't go under it. Must go through it. It has been longer than I had intended since my last update! Mostly because I have been spending a lot of time living this new life and loving this new body! But also because I have spent a good amount of time since the end of June with gout. So perhaps that's where I'll start. In my last post I updated that I had been down and out with gout. Since that time, I have had an attack about every two weeks. Each time it has been bad enough that I have been unable to walk without crutches or a knee scooter. The last really bad attack I had was in both feet, both ankles, and my right hip. Pain like that and being so limited with mobility definitely took a toll on my spirits. Even being so thrilled with how great I am feeling otherwise, I have spent a good amount of time being really frustrated and sad the last three months. I am very grateful that I have a job and employer who has been understanding through the whole ordeal and has given me the flexibility to work from home as needed until I am past all of this. It's been a major blessing. The good news is, that I am learning what symptoms prior to an attack feel like and I have Colchicine (a medication for acute attacks) on hand to take as soon as I feel the onset of symptoms. It seems to help decrease the severity and length of the attacks. I titled this post "The Bear Hunt" in reference to the well-known children's song. A sweet friend and colleague of mine sent me the nicest message the other day saying that as she has observed my journey over the the last few months, I reminded her of the song. "Can't go over it, can't go under it, must go through it." I am not sure she realizes how much that meant to me. But it was something I needed to hear and given at a time I needed it most. So no matter what comes my way I will keep on keepin' on and go through it with tenacity, gumption, and a grateful heart. Okay...onward to the exciting stuff! Transformation Progress It's been nearly 12 weeks since surgery and I am amazed and the transformation I am seeing. As of this morning, I am officially down 78 pounds and at the lowest weight I have been in the last 15 years. I am also down four sizes. My closet is dwindling rapidly. I am trying not to buy too much new because I know it won't be long before I am out of it. On the occasion where I have had to buy a new top or pants, I continue to be shocked at the size I actually need. I will typically grab two sizes too big off the shelf and think to myself "there's not way this will fit." And I am right. It doesn't fit because it is too BIG. It's definitely a great feeling.
I have also had a significant number of "non scale victories." Here are just a few:
0 Comments
Greetings! Today marks nearly 5 weeks post-op and it is time for another update! I have so many things to share with you on this post so stick with me to the end! Energy Changes Every day since surgery I feel like I wake up and see someone different in the mirror. I don't really recognize it as weight loss though. I look in the mirror and see eyes looking back at me that aren't exhausted. I see skin looking back at me that looks younger and brighter. I see a woman looking back at me who is on possibly the hardest journey of her life and crushing it. At about 3 weeks post-surgery I found that my energy levels had skyrocketed. I had an extremely busy first week back to work after surgery and I anticipated that I would come hope completely exhausted. Instead, I found that I had more energy than I knew what to do with. I used to get home from work and the thought of cooking dinner and cleaning up was almost more than I could handle. I was tired ALL the time. But at 3 weeks out, I began to have energy to come home and cook dinner, do a little cleaning, run errands, and complete any other number of activities! I even have the energy to workout again. Getting home from work and accomplishing so much yet still having the energy to lace up my sneakers and get a workout in is a feeling that I have missed so much. I really didn't realize how low I had gotten. I had just accepted that constant fatigue was my new life and being tired all the time was my new normal. Above anything else, even if I don't lose a single ounce more than I have, this alone makes this whole process worth it. My sleep pattern has also been totally shaken up for the better. I used to be ready to crawl into bed at 9:00pm and wake up at 7:00am still exhausted. Now, I am going to bed around 11:00pm and waking up at around 6:00am with little issue. Confidence Changes I am not sure that I can attribute this next part to my surgery per se. However, I think that it is the experience I have had that has given me a new platform to be an advocate for myself and others. This part of me was always there. But I think because of my journey the spark has been rekindled and I have a new fire inside of me. First, I am taking a more specific look at my feelings and my needs. Specifically as it relates to my career and professional growth. I have found a new spirit in myself to be my own advocate, ask for what I need, and speak up when something is bothering me or I have an idea or opinion. I have a bad habit of just "going with the flow" or being overly accommodating to my own detriment. Thought I still have work to go in this area, I have had a few notable moments recently that have made me really, really proud of my progress. This journey, though rewarding, is NOT for the weak. It is hard. It is REALLY hard. But in doing this really hard thing, I have realized that I CAN do hard things. And I AM worthy of living my best life. And I find myself taking more steps daily to be the driver in my own life...and not a passenger. Second, I have also undertaken a personal mission to advocate with my employer for weight loss surgery to be included as part of our healthcare plan. Currently, all weight loss surgery, regardless of the medical need, is written as an exemption to our policy. Though pushing for this change now won't help me (I was a self-pay patient), I hope that it will be able to help others. I sent an email to a few of our executive leaders two weeks ago providing an overview of the health benefits of weight loss surgery and shared my personal experience thus far. I asked for an audience with them to open a dialogue about getting our policy revisited and reconsidering weight loss surgery as a policy exemption. This is very common though more and more policies are being revised to include it. Though I don't know where it will go, I am happy to say that they were very receptive to my request and I have a meeting with them on Friday to discuss it further. My employer is very invested in the holistic wellness of their employees and I am pleased that at a minimum, we're starting a dialogue! Body Changes Okay y'all...I still have to tell you about a few important things before we get to this. So...THIS IS A TEASER SECTION! Keep reading. It'll be worth it I promise. Eating Setbacks For the first few weeks after surgery eating wasn't too big of an issue. There were things I couldn't tolerate but overall eating wasn't a huge deal. When you find a food you can't tolerate, at least for me, it is painful. You feel like you need to vomit but can't. Your body starts creating excess saliva and mucous to get the food down and you start salivating like a rabid dog. My nose also runs like a faucet. It is typically a pretty miserable 20 minutes and then it passes. I have had this happen about 5 or 6 times since surgery. It's really hit and miss and I can't predict what I will be able to tolerate and what I won't. Aside from the discomfort of eating a food that doesn't sit well, my biggest setback food wise lately is that eating has become like a chore. I actually dread it. Nothing sounds good. Nothing tastes good. Food has completely lost all joy for me. I hear that it gets better, but right now it is hard. It is really hard. This was an unexpected development for me. I knew I would only be able to eat small amounts moving forward but I didn't anticipate that food would lose its appeal altogether. Physical Setbacks On Wednesday June 26th I came home from work and got on the treadmill. I got my workout in and then noticed afterward that my foot was really hurting. I thought maybe I had stepped wrong or just put to much pressure on it during my workout. The next day it was really painful and I was convinced I had somehow sprained my foot. On Friday evening, I went to visit my parents and as the night went on, I was having more and more pain and it was getting progressively harder to walk. I ended up staying the night because it got late and I wasn't confident I could push the gas pedal on my car to drive home. Saturday morning I woke up and was still in a lot of pain but was able to hobble to my car and drive myself home. By the time I made it to home, I could barely walk into the house. The next 24 hours were filled with the worst, unrelenting pain I have ever had in my entire life. I finally figured out on Saturday that I hadn't sprained my foot at all. I have gouty arthritis and was in a full blown gout attack. I have had elevated levels of uric acid for at least two years now but never really had a bad gout attack. In retrospect, I do think some of the pains that I have had in my ankles and knees over the last two years were actually gout. I had always just attributed it to my weight or that I had twisted a joint funny and didn't realize it. But now I am confident that I was having a mild gout flare. I have watched my dad suffer with gout my entire life but never really understood the pain he was going through until now. By Saturday mid-day I was in so much pain I was delirious. I couldn't walk. If I needed to make a trip to the bathroom I had to crawl on my hands and knees. I called my surgeon's after hours number and was able to talk to the surgeon on call. He said that it was fairly common for individuals with gouty arthritis to have a flare up after surgery due to the rapid weight loss. He called me in a prescription for colchicine that I had Ken pick up and started to take immediately. I also had some liquid hydrocodone that I took Saturday and Sunday to help minimize the pain. However, I would only get about 20 minutes of mild relief through that. The pain was no joke and not even hydrocodone could really touch it. Over the next 5 days the colchicine helped to reduce the swelling in my foot and break up the uric acid in my joints. I was unable to tolerate any weight on my foot at all (I ended up having Ken pick up some crutches so I didn't have to crawl) until Thursday afternoon. Today, I am 8 days into this flare up and still have pain. I am able to walk so I am grateful for that. The constant pain is managed as long as I am not on my feet for too long. *One huge disclaimer that I want anyone considering this surgery to be aware of is that after surgery you cannot take NSAIDs (non steroidal anti inflammatory drugs) anymore for the rest of your life. They are too hard on your new digestive system and you are at an increased risk for gastric ulcers. Even two doses is enough to eat a hole through your new stomach pouch. So, my option for pain relief now is Tylenol. This has done the trick so far until the gout attack. So for anyone with arthritis who typically relies on NSAIDs to manage arthritic inflammation, you will definitely need to discuss this with your doctor if you are considering surgery.* Body Changes Part 2!
Okay here is the status update on my body transformation! My surgery was on June 3rd. I weighed myself on July 4th and I am officially down 34 pounds! I can definitely feel the difference in my body. Some before and after photos are posted below. Thanks for reading and supporting me in my journey! I will update in another two weeks! Hello everyone! Today is nearly two weeks post-op! This blog post will take us from the day after surgery through today.
Surgery Recovery and The Best Mom The night after surgery I slept really, really well. I was prescribed liquid codeine and took it before bed to help with pain. I stayed at my mom and dad's house for two days following surgery. I was really worried about falling asleep because of the scary first night I had, so I stayed with them so my mom could watch me that night and take care of me. I also stayed because I knew there was no way I was going to be able to handle all of the bumps on the car ride back to my house because I-15 is torn up and an absolute mess. Ken was super supportive and came down to see me when he was off work. I was grateful for a good night's sleep and the comfort of knowing my mom was there to watch me in case I got into trouble during the night. But I am happy to report that things were just fine and the hospital potassium hiccup was a one-time fluke. Over the next two days, my mom took really good care of me and I am so grateful for her. Her support and care made a rough couple of days so much easier. Gas Pains, Liquids, and The Potassium Conundrum The first two days after surgery I focused mainly on walking to alleviate the gas pain I had, which was not fun. I've never had pain like that before and I don't really know how to describe it. During a laparoscopic procedure, they essentially blow you up like a balloon, and it took about 5 days before I felt like all of the air was out of my body. For me, it settled in right below my sternum and shoulder blades and walking was really the only thing that helped it go away. I needed the prescription pain meds I was given and chewable Tylenol for breakthrough pain until Wednesday evening, and then I didn't need to take anything after that. I also focused on getting in my meals and fluids over the first few days because it definitely takes some intentional work and time. My meals consisted of chicken broth and sugar-free jello for the first two days after surgery. After that I was able to move to full liquid which included yogurt, string cheese, and cottage cheese. Each meal was limited to four tablespoons. I also worked really hard to get in a full 64oz of fluid. It's a lot of small sips which has taken some getting used to because I am typically a guzzler. Ice water was impossible at first (and still is). The cold liquid caused my insides to spasm and was actually pretty painful. So I moved to room temperature liquid and it got a lot easier to get all that liquid down. I also had to continue taking potassium supplements which I was NOT looking forward to. They were so painful to swallow in the hospital and I did not want to go through that again. The pain after gastric bypass when you swallow too much of something at one time is like a massive cramp right under your sternum. And depending on what you swallow it can last anywhere from a minute to thirty minutes. So needless to say, I wasn't keen on trying to take them anymore. We called the pharmacist because the prescription for the potassium said not to chew or crush (eye roll), but after talking to them they said that it was ok to dissolve the pills in some warm water. So we tried that...but the potassium pills don't really dissolve completely. They dissolve down into large granules that settle in the bottom of a glass of water. So after three attempts to drink it down out of a shot glass (remember I can only drink about an ounce at a time), we needed another solution. I had the idea to draw it all up into a syringe and try squirting it in my mouth instead. However, on the first try using the syringe, all of the water squirted into my mouth but left all the potassium as a plug in the syringe. Fail! So now my mom decided to give it a try. I opened my mouth, she took aim, and she hit the plunger really hard to try and get it all out. Oh and it came out....forcefully! It shot into my mouth, hit the back of my throat, and gagged me. Some of it sprayed in my hair and on my face, and some of it sprayed back on my mom. We both about died laughing (I was laughing and choking) and decided it was time to give up on the potassium! So...I just stopped taking it. I was grateful for the much needed laugh, though belly laughing like that after surgery hurts quite a bit...even if you are holding your stomach. :) Emotions and Head Hunger Here me when I say this, I wasn't at all prepared for the emotions that I would have the week after surgery. Everything just felt really raw and at the surface. I would tear up and cry for no reason. I was also working through a lot of head hunger. As an emotional eater, when these emotions surfaced, I didn't know how to manage them because food was no longer an option. It was now, for the first time, that I confronted the fact that my relationship with food as I knew it was over. Forever. I absolutely knew this going into surgery...but it didn't REALLY hit home until my first meal of chicken broth and jello. Gone are the days of a plate of spaghetti for dinner. Gone are the days of a cheeseburger and an order of fries. Gone are the days of an ice cream cone or milkshake as a Friday night treat. Hell, gone are the days of a big cobb salad or a piece of corn on the cob. Honestly...I found myself grieving with that realization for the first several days. Add that to the fact that I had just undergone major surgery. In retrospect, I guess some raw emotions should have been expected. Following surgery you are in pain, you are exhausted and emotional, you're hungry (legitimately) but you also have head hunger. It's a lot to deal with. Fortunately, when I was able to move up to full liquid, and the gas pains had subsided, a lot of this went away. The cravings, the head hunger, it all got better. But it's not gone forever. And I have had moments here and there. This is and will be the biggest challenge to this new life. Because not only does my relationship with food change, but it changes in a way that only those who have had weight loss surgery can really understand. I will never consume food again in the way that the general population does. My anatomy is physically changed so that how I eat and what I eat will be altered forever. It's worth it...but that's heavy. Especially in the beginning. Post-Op Follow Up Ten days after surgery I had a follow up with my general practitioner. His name is Jordan Roberts and he is located in the Holiday Family Practice at Granger Clinic. He is absolutely the best doctor I have ever had. So if you are looking for someone new I highly recommend him. Anyway...ten days post op, I followed up with Dr. Roberts to check my blood pressure, potassium, and incision sites. Drum roll.....
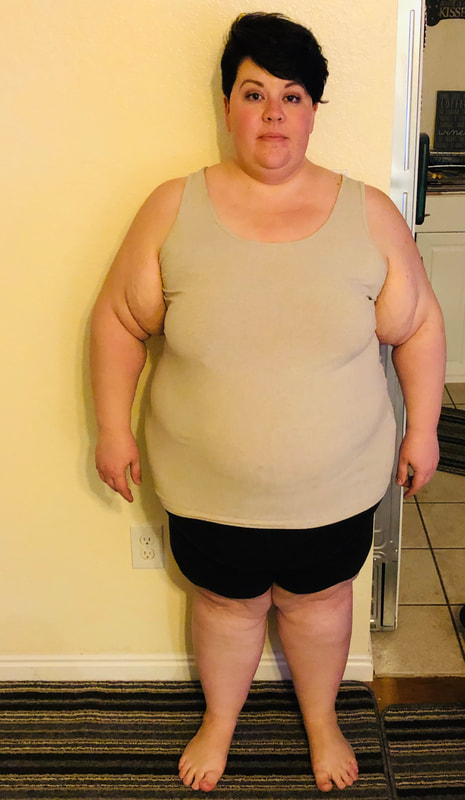
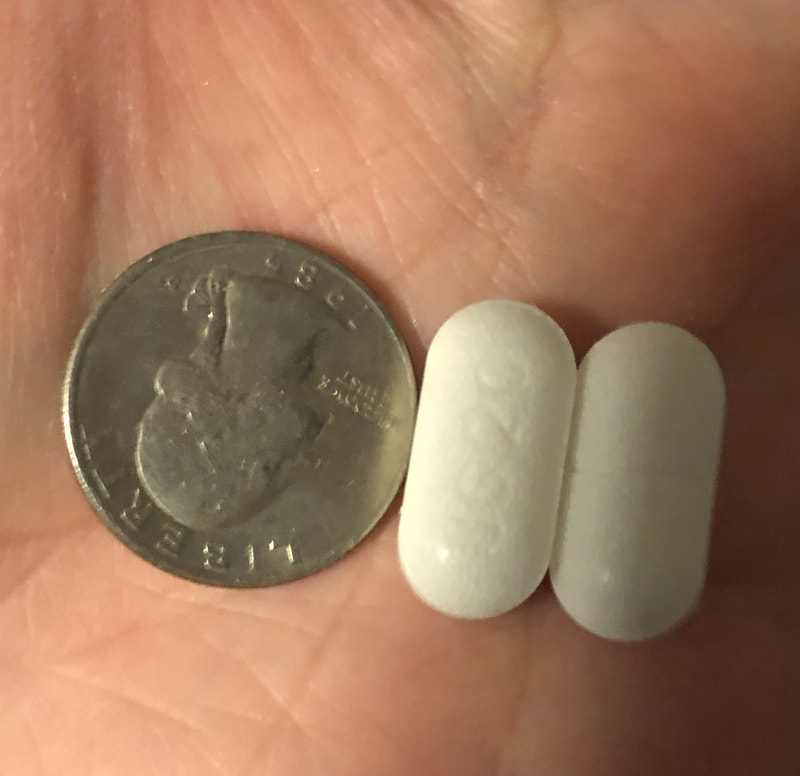
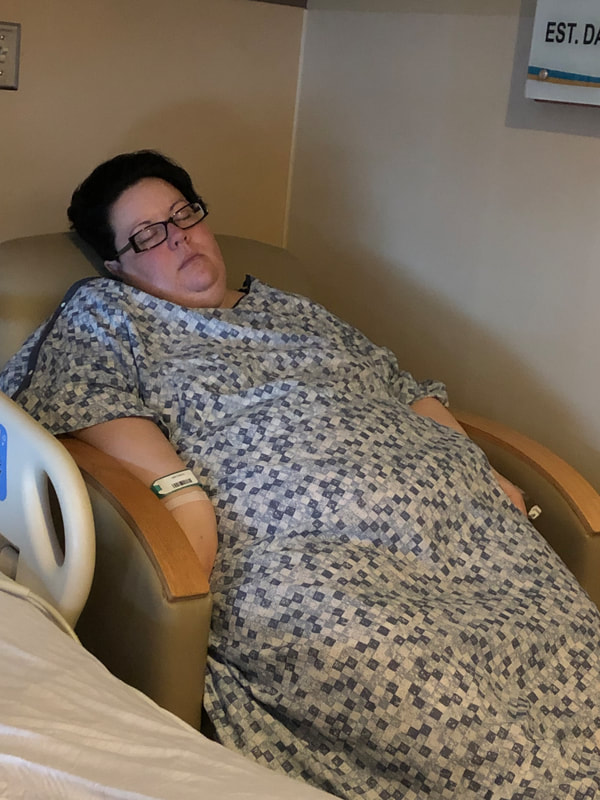
Today officially marks 5 days post surgery! This is the first day I felt up to sitting down and typing up a post so I have a bit of catching up to do! This post will take us through the night before surgery through my discharge at 1 day post-op. Pre-Surgery Jitters and "Before" Pictures The night before surgery was the first time I really started to get any nerves. I was mainly nervous about getting to the hospital, having them put me under, and then deciding not to do the surgery. It was a bit irrational in retrospect, but I was so anxious to get things underway I was really worried that something would happen to postpone the surgery or make it so that it couldn't happen. Jitters aside, I was actually able to sleep really well that night. As I was getting ready for bed, I showered and washed with the antimicrobial wash as instructed, and I decided it was finally time to take my dreaded "before" pictures. I put them off for a long time, partly because I didn't want to see them. But truth be told, I mostly put them off because I didn't want to feel like the Kacey before surgery was any less worthy, any less loved, or any less me than the Kacey after surgery would be. So I struggled with whether or not to even take them. In the end, I decided to do it because I want to be able to see my progress along the way. I want something to look back on and see how much my body has changed...my equally loved, equally worthy, equally me body. So here I am taking a majorly vulnerable and scary step by sharing them with all of you who are reading. Surgery Day The morning of surgery I woke up and showered again with the antimicrobial soap as instructed. I also had to "shower and go" meaning no hair styling or makeup. And anyone who knows me well knows that meant I died a little inside! Ken and I hit the road at 7:30am to make sure we arrived at the hospital by 9:00am. We met my mom there at the front doors and walked in together up to the 5th floor for surgery check in. Right when we got there we were shown to a room where I changed out of my clothes and into my hospital gown and socks. Shortly thereafter, they placed my IV line. I was absolutely amazed at how quickly they did it because normally everyone struggles to hit my veins. They used a vein finder and lidocaine to numb the site so it was easy peasy and pain free! They also gave me an injection of heparin and one of the medications (atenolol-chlorthalidone) that I take on a daily basis. Keep this in mind because it gets pertinent later! We waited for probably 30 minutes after that for someone to come and wheel my bed down to the surgery waiting area. The man who came for me was named John and he was simply wonderful. He made me trade the headband I was wearing for a surgical cap and we were on our way! He joked with me and kept the conversation friendly and flowing. It went a long way to keep me, Ken, and my mom all calm and relaxed. Once we got to the surgery waiting room, I was greeted individually by the operating room nurse, my surgeon, and the anesthesiologist. It was all a really great experience and I felt like I was in good hands. The anesthesiologist and nurse did the most to settle my nerves. My nurse let me know she also had gastric bypass five years ago and that it was the best decision she has ever made. So that was comforting! The anesthesiologist let me know he would be responsible for monitoring my vitals the entire time. Putting a face to the person who would be responsible for something so important was really comforting. I asked him who would be in charge of making sure I stayed breathing after surgery (this was one of the fears that manifested for me that morning) and he reassured me that I would be monitored very, very well by my recovery nurse. After the introductions, the anesthesiologist wheeled me to the operating room where I then transferred onto the operating table. I was quickly introduced to the surgical team. I remember looking to my left and smiling at the surgical staff and that was the last thing I remember. They didn't let me know when they were ready to put me under...so one minute I was smiling and present...and then I wasn't. The next thing I remember was waking up really, really groggy and moaning a lot. I was in pain but didn't understand why. It took me a minute to register where I was, what had happened, and that I was out of surgery. I don't remember a whole lot about being in the recovery room. I remember the nurse telling me I was ok and that they would be giving me something to help with my pain and I would get relief soon. I also remember her handing me the PCA pump that allowed me to give myself doses of Dilaudid. I do remember asking the nurse at one point "am I skinny yet?" but that's about all I really remember from the recovery room! I do remember being wheeled out of recovery into my own hospital room and seeing Ken and my mom there waiting for me. It was a big comfort to finally see their faces. All in all, the surgery itself lasted about an hour and I was in recovery for about the same amount of time, so I was comfortable in my own room at about 11:45am. By this point I was feeling great (thanks anesthesia and dilaudid!) and still coming out of anesthesia...but I thought I had it fully together. The picture below is evidence otherwise! Once I was in my room, I was greeted by my care staff for the day including the CNA and nurse who would be caring for me over the next several hours. They were absolutely amazing. At about 12:30pm they started having me take small sips of water. I was allowed 1oz every hour. My mouth was really, really dry so they gave me some oral sponges to help and let me have a few ice chips as well. Drinking the water initially out of surgery didn't hurt but definitely caused a cramping discomfort when I swallowed. My throat was also sore and a little hoarse from the intubation tube. It was about this time that I also "met" my neighbor in the room next to me. She was an elderly woman who kept calling out "help me" at the top of her lungs during the times she was awake (which was a lot). It was absolutely heartbreaking and something I will remember forever. Around 3:00pm I was feeling great and ready to get up and take my first walk. My mom was there with me and helped me do 4 laps around the nurse station. Walking is absolutely essential after surgery to help dissipate the gas that they pump you full of so I was determined to do it. On our walk, I noticed my ears started to feel like I was under water because my hearing sort of got muffled. It passed pretty quickly so I didn't mention it at all. At 7:00pm I was ready to take another walk before the nightly nursing staff change. My mom went with me again and we did 5 laps around the nursing station. I needed to pause in the middle because my head felt like I was under water again and my hearing became muffled. After stopping for a few minutes it cleared again and we walked back to my room. Things to this point had been absolutely fabulous, I felt great, and my care team had been amazing! Oxygen was good, pulse was good, blood pressure was good, and I felt fantastic. By this time I was just ready to hit the hay and get some rest so Ken and my mom headed home and I put on a tv show to fall asleep to. This is where things start to get a little fuzzy for me. I remember the alarm on the monitor that was checking my vitals started to beep incessantly. Every time I was just about to fall asleep it would go off again. My poor little neighbor was also having a struggle and continued to cry out for help continuously through the night. I remember looking back at the vitals monitor and seeing my oxygen level in the low 80s and my pulse rate at 46. It was at that point that I pushed the call button for the nurse and the CNA came into take my vitals. When the CNA took my blood pressure it was 90/46. I remember asking her if it was anything to be worried about and she told me no since I hadn't had any blood in my stool (?) and my drain looked fine. Through the night, my vitals continued to be really volatile. My pulse and oxygen would come back up to normal levels (Pulse 75 Oxygen 98) and then drop significantly (Pulse 40s Oxygen low 80s). A few hours later when the nurse came in to take my vitals I asked again if it was anything to worry about. She said that it was probably the dilaudid. My brain was fuzzy so I didn't push any further but I knew something was off. I was having a hard time breathing and had to concentrate on each breath in and each breath out. Because of this, I had sat myself completely upright in the hospital bed. At one point, I tried to recline it back down but it wouldn't work. Three different people came in to look at it and couldn't fix it. I spent the rest of the night sitting upright, focusing on breathing, with my alarm going off about every 10 seconds. At about 5:00am the next morning I had the sense to finally text my mom who immediately came up to the hospital. Before she got there, they drew a blood sample and let me know my surgeon would be coming in shortly to talk with me. My mom and the surgeon walked in at about the same time and that's when I found out that my potassium had dropped to critical levels in the night. They believed it was due to the atenolol-chlorthalidone that I had been taking prior to and the day of surgery. At this time the nursing staff changed again and I was prescribed potassium supplements to take. They were HUGE pills and really hard to swallow with my ounce of water allotment. It was extremely painful but I finally got them down. My mom made sure the new care team fixed my bed so I could finally lay down and also had them change the sensitivity on my monitor so that the alarm beeping would stop. I was finally able to get some sleep in the chair in my room. They took more blood and tested it to make sure my potassium was back in a safe range after giving me a second dose of potassium pills (4 total). About two hours after the potassium supplements my vitals began to stabilize. Over the next several hours my mom and I just talked and worked on my water sips and breathing exercises. Things started to turn around and I was doing really well. The head nurse for the floor (I believe she was over quality control) also came in and asked me for feedback from the night. I was able to share the night's events with her and she was a great support in making sure I had everything I needed for the last several hours of my stay. At about noon my levels had stabilized and things looked good so they let me know that I could be discharged around 4pm. Just prior to discharge, my new nurse Jose came and took the staples out of 5 of my incision sites. He removed the drain from my 6th incision site. That drain was a trip. It freaked me out having it hanging out of my body. I didn't actually realize until after it was removed that it was easily 2 feet of tubing that was inside me...maybe more. Sometimes ignorance is bliss!
I was discharged at 4:00pm and still a bit shaken from the night's events so I ended up going home with my mom where I would spend two days (I'll post about this tomorrow). I don't recall much from the drive home because I slept in the car. My pain was well-managed and I was grateful to be heading to the comfort of home! My surgery is scheduled for Monday, June 3rd. As the day grows closer, I am getting more and more excited about the journey and can't wait to get started. I have been following a lot of support groups on Facebook for a while now that have been instrumental in helping me make the best and most informed decision I can about my way forward. I think all of the positivity and support that they provide has definitely kept any nerves at bay.
I have been contemplating weight loss surgery for some time now. One of the biggest reasons I have put it off for so long was because of the stigma that surrounds it. When my PCP mentioned it to me nearly 5 years ago I was mortified and shut the idea down immediately. Why? Well, if you talk to enough people about weight loss surgery you will find many people see it as an "easy way out." I bought into this philosophy about myself for a long time. The truth is that weight loss surgery of any kind is absolutely NOT an easy way out. It is hard. And the life change that accompanies it is significant. So to view weight loss surgery as an "easy way out" is at best uninformed. There is nothing easy about it. And to those who have struggled with your own weight, I see you and I know how hard it is. If you are contemplating this journey for yourself, or have written it off hastily, I urge you to do your research and shut that narrative down. Because simply put, it isn't true. Okay...onward! My surgeon requires a two week pre-op diet that consists of meal replacement shakes during the day and a small, high-protein meal (around 350 calories) in the evening, not to exceed 1,000 calories per day. The purpose of the diet is to prepare your liver for surgery because even a small drop in weight can cause the liver to shrink and make it easier to do the surgery. It hasn't been too difficult so far. Day 2 and 3 were the hardest. I definitely had real stomach hunger for those two days, and from there on out, it was largely a mental game. Sugar-free popsicles have been a life saver! I have my last surgery preparation class and pre-op appointment tomorrow and then surgery on Monday! I plan to take pictures this weekend to share and then weekly thereafter to document my progress. So, this is it for now! Thanks for reading and thanks for following along. Here we go. |
Site powered by Weebly. Managed by Hostgator
















 RSS Feed
RSS Feed